Red Light Therapy for Teeth and Gums
Red light therapy might not be the first thing that comes to mind for teeth and gum care, but it has become a growing area of interest in dental research.
Photobiomodulation (PBM), also called red light therapy, is being studied in medical and dental settings for wound healing, inflammation, and soft tissue healing.
In dentistry, low-level laser therapy (LLLT) has been used in clinical settings in relation to gum disease, post-procedure discomfort, and healing after oral surgery.
More recently, at-home oral care devices have made red light therapy more accessible, especially for people exploring red light therapy for receding gums.
Red light therapy for oral health has drawn attention not just because of product marketing, but because of how photobiomodulation interacts with living tissue. The mouth contains highly vascular soft tissue and researchers have examined how specific wavelengths of light interact with cells in these areas.
When those wavelengths are applied under the right conditions, studies have reported measurable biological activity at the cellular level.
Key Takeaways
- Red light therapy (photobiomodulation) stimulates cellular repair in gum tissue by energizing mitochondria — the same mechanism used in professional dental laser treatments.
- Dental research has examined red light therapy for gum inflammation, bleeding, tooth sensitivity, and healing in certain settings.
- Low-level laser therapy (LLLT) is already used in some clinical dental settings, while at-home devices apply the same general photobiomodulation concept.
- Red light therapy is not a replacement for brushing, flossing, or professional cleanings — it works best as a supportive tool in a complete oral health strategy.
- Keep reading to find out which wavelengths are most relevant for gum tissue — and why most people using red light at home are missing this critical detail.
How Red Light Therapy Works Inside Your Mouth
Red light therapy delivers specific wavelengths of light, usually in the 630nm to 850nm range, straight to living tissue. Unlike UV light, which can harm cells, red and near-infrared wavelengths are absorbed by tissue without creating damaging heat. This leads to a photochemical reaction within the cells themselves.
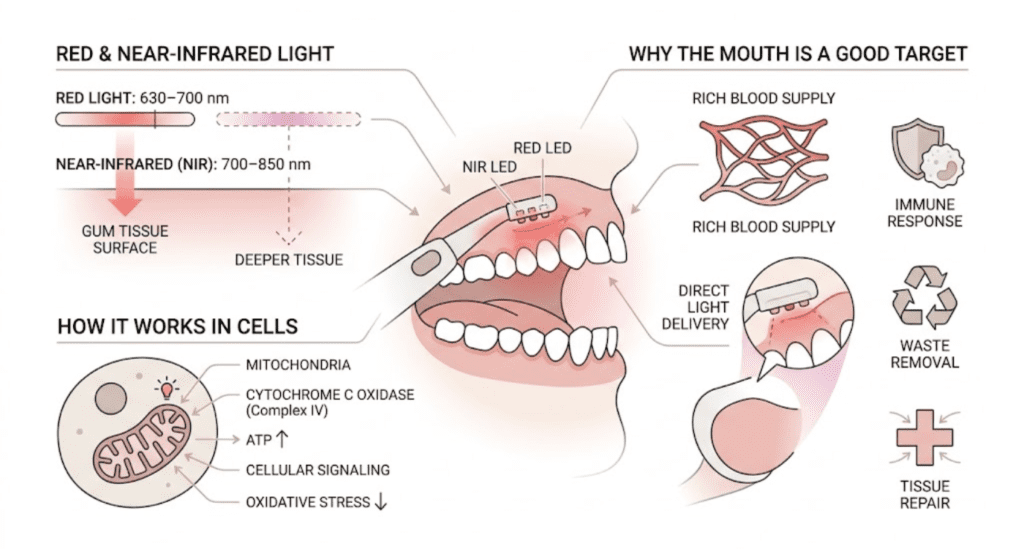
The Effect of Red and Near-Infrared Wavelengths on Tissue
Red light comes in many forms, but only certain wavelengths are commonly discussed in photobiomodulation research.
There are two main categories: Red light (630–700nm) can penetrate the surface layer of gum tissue and may support reduced inflammation and surface healing. Near-infrared light (700–850nm) can penetrate deeper into oral tissue and may reach areas below the gumline, including deeper supporting structures.
That is why some oral care devices use both red and near-infrared wavelengths rather than red light alone. Because the tissues in your mouth sit at different depths, wavelength choice can affect how a device is positioned and used.
How Mitochondria Contribute to Gum and Tooth Healing
One of the main ways photobiomodulation is thought to work is through the mitochondria, where red and near-infrared light may influence cytochrome c oxidase, ATP production, oxidative stress, and cellular signaling.
In gum tissue, these effects are being studied for their potential role in healing, collagen activity, inflammation, and tissue response, which is why red light therapy is often discussed as a supportive tool for oral health.
Why Red Light Therapy Works Well for the Mouth
Our mouths are one of the best places for photobiomodulation to work because they are full of blood vessels. When light helps support blood flow in the area, it may also help support immune response, waste removal, and the tissue repair process.
It also helps that the treatment area is easy to reach. When a device is used inside the mouth, there is also less tissue between the light source and the treatment area.
Compared with treating deeper tissue through the skin, intraoral use allows light to be applied more directly to the gums and other soft tissues.
The Advantages of Red Light Therapy for Gums
Some of the most commonly discussed uses of red light therapy in oral health research involve the gums.
Gum tissue is biologically active and constantly exposed to bacteria, inflammation, and everyday mechanical stress, Red light therapy tackles many of the fundamental causes of gum degradation.
- With regular use, some people may start noticing less redness and swelling along the gum line over time
- As the inflamed tissue becomes less reactive, brushing may feel more comfortable and bleeding may lessen
- The amount of bacteria near the gum line may decrease because of the antimicrobial properties of certain red light wavelengths
- The activity of inflammatory cytokines slows, which may help protect the connective tissue below the surface of the gums
Less Gum Inflammation and Bleeding
When your gums are inflamed, the condition is called gingivitis, which is the earliest stage of gum disease and is often marked by redness, swelling, and bleeding during brushing or flossing.
Gingivitis is considered reversible with appropriate dental care and good oral hygiene, but ongoing inflammation can contribute to changes in the tissues supporting the teeth.
Red light therapy is being studied as an adjunct in periodontal care because it may influence mitochondrial activity, ATP production, oxidative stress, and inflammatory signaling.
In dental research, low-level laser therapy has been associated with reductions in some markers of gingival inflammation in certain treatment settings, though results depend on the condition, protocol, and device used.
Improved local blood flow is another key factor. By increasing blood flow to inflamed gum tissue, the body can more quickly remove inflammation-causing substances and deliver fresh immune cells to combat the bacteria causing the initial irritation.
Many people see a decrease in bleeding during brushing as one of the first signs of improvement. This is one of the earliest and most dependable signs that the gum tissue is moving from a state of inflammation to a healthier state. If your gums bleed regularly when you brush, that’s not normal, and it’s one of the clearest signals that your gum tissue needs support.
Less Gum Recession
Gum recession occurs when the tissue that surrounds and protects your teeth starts to pull back, exposing more of the tooth root. It can happen slowly, often without pain, until sensitivity, aesthetic changes, or bone loss make it impossible to ignore. Once gum tissue recedes significantly, reversing it typically requires surgical intervention.
While red light therapy won’t bring back gum tissue that’s already receded, it may help support the health of the remaining tissue by promoting a healthier inflammatory response and normal healing activity in the gums.
Speeding Up Healing After Gum Irritation or Injury
Whether it’s a cut from flossing too hard, irritation from a dental procedure, or a stubborn canker sore, the mouth endures a lot on a daily basis. Red light therapy has been studied for how it may support soft tissue healing, in part through effects linked to fibroblast activity and collagen production.
Fibroblasts are the cells involved in building the collagen framework that helps repair and support tissue structure. In dental and oral surgery research, low-level laser therapy has been associated in some settings with improved healing outcomes and reduced post-operative discomfort, though results vary by treatment type and protocol.
How Red Light Therapy Helps Your Teeth
Red light therapy is often associated with gum health, and that’s what most of the research focuses on. However, the benefits of red light therapy go beyond just the gums. It can also help with tooth sensitivity, the health of the tooth root, and the structures that support the teeth.
Teeth do not function in isolation from the tissue around them. They are connected to the jawbone by the periodontal ligament, a living tissue that responds to inflammation, bacterial pressure, and mechanical stress.
By supporting the health of the surrounding tissue, red light therapy may help support the structures that contribute to long-term tooth stability.
Your teeth rely on healthy gums and supporting bone for stability, so any approach that helps support that foundation is part of the broader conversation around long-term oral health.
Less Sensitive Teeth
One of the most common dental issues is tooth sensitivity, which is a sharp, sudden pain that can be caused by hot drinks, cold air, or sweet foods.
This issue affects a large number of adults. It usually happens when the dentin layer of the tooth is exposed, either because the enamel has worn away or the gums have receded. This allows outside stimuli to reach the nerve inside the tooth.
Red light therapy has been studied as a non-invasive approach for dentin hypersensitivity, which is why some dental professionals include low-level laser therapy in sensitivity care before moving to more invasive options.
Helps with Remineralization
Remineralization is the natural process in which minerals such as calcium and phosphate are redeposited into weakened enamel during the earliest stage of enamel damage.
This process depends heavily on the health of the saliva, the oral microbiome, and the surrounding tissue environment. Red light therapy contributes to this process indirectly by reducing the bacterial load near the gumline and improving the tissue health of the structures surrounding each tooth.
There is also growing interest in whether photobiomodulation may influence odontoblast activity. Odontoblasts are the cells that line the inner surface of the tooth and produce dentin, and this remains an emerging area of research rather than an established clinical benefit.
What Does the Science Say About Using Red Light Therapy for Dental Health?
Red light therapy is not a new idea in dentistry. Under terms like low-level laser therapy (LLLT) and photobiomodulation (PBM), it has been studied in relation to gum disease, oral surgery recovery, pain, inflammation, and wound healing.
The research is promising, but it is more accurate to say the evidence varies by application, device, wavelength, dose, and treatment protocol.
When the right parameters are used, red and near-infrared light have been associated in dental research with support for gum tissue health, healing, and pain management, which is one reason these treatments have traditionally been delivered in clinical settings.
How Dental Professionals Use Low-Level Laser Therapy
For years, dental professionals have used low-level laser therapy (LLLT) in clinical settings, including as an adjunct to scaling and root planing, as well as in research around oral surgery recovery, aphthous ulcers (canker sores), and temporomandibular disorders (TMJ).
Studies have shown that when laser therapy is added to the treatment, the results are significantly better than with mechanical cleaning alone. It’s also used for healing after surgery, treating aphthous ulcers (canker sores), and managing pain in the temporomandibular joint (TMJ).
That long clinical history does not mean every use is equally proven, but it does show that photobiomodulation is an established part of the dental research conversation rather than a new at-home trend.
How NASA’s LED Red Light Research Contributed to Wound Healing
Some of the early attention around LED light therapy came from NASA-linked research into how specific wavelengths of light might affect cell growth and wound healing, originally in the context of space-related health and plant-growth experiments.
That work helped draw wider medical interest to light-based healing applications and contributed to the early development of photobiomodulation research.
Rather than proving every modern use of red light therapy, the NASA work is better understood as part of the early research history that helped support the biological plausibility of using red and near-infrared light in wound healing and tissue repair. Dentistry later became one of several clinical fields where photobiomodulation was studied further.
How to Use Red Light Therapy for Teeth and Gums at Home
Red light therapy is an easy at-home treatment for oral health, but it’s important to be consistent and use the right device to see real results. This isn’t a once-a-week treatment. The cellular benefits of photobiomodulation build over time with regular, repeated exposure.
Most protocols recommend daily red light therapy sessions, ideally paired with your existing brushing routine so it becomes automatic rather than an extra step you have to remember.
The timing of your red light therapy is also key. It’s best to use red light therapy after you’ve brushed and flossed your teeth so that your gums are clean and there’s nothing to block the light from reaching the tissue. Some at-home devices are built right into toothbrush heads, making it easy to incorporate into your oral care routine. Other devices are standalone mouthpieces that you wear for a certain amount of time, usually between 5 and 10 minutes, after you brush your teeth.
How to Use Red Light Therapy at Home for Gum Health

- Brush your teeth for 2 minutes with a soft-bristled toothbrush, making sure to brush along the gumline.
- Floss to remove any food particles from between your teeth and just below the gumline before you use the light.
- Rinse your mouth to remove any loose food particles so that the surface of your gums is clean.
- Use your red light oral device as directed. If you have a mouthpiece device, you’ll usually use it for 5 to 10 minutes. If you have an integrated device, you’ll use it while you brush your teeth.
- Use the device every day. You’ll get the best results if you use the device consistently.
It’s important to remember that your mouth has different surfaces. You have front teeth, back teeth, and gums. When you use a red light device, make sure the light reaches all of these surfaces.
It should reach your whole mouth, not just the front teeth that you can see easily. Devices that are made for oral use are designed to do this. That’s why these devices are better than generic handheld devices for this use.
What You Should Look for in a Red Light Dental Care Device
Not every red light device that is marketed for dental use delivers clinically relevant wavelengths or adequate energy density. When evaluating a red light dental care device for home use, these are the specific features you should prioritize:
- Wavelength range: Look for devices emitting in the 630–660nm (red) and 810–850nm (near-infrared) ranges. These are the windows with the strongest evidence for tissue healing and inflammation reduction.
- Full-arch coverage: A mouthpiece or integrated toothbrush design that reaches both upper and lower arches simultaneously is far more practical than a single-point device.
- Irradiance (power density): The device needs to deliver enough energy to the tissue to produce a photobiomodulation effect. Too low and it’s decorative, not therapeutic.
- Safety certification: Look for FDA-cleared or CE-marked devices that have been tested for oral use specifically.
- Ease of integration: The best device is the one you’ll actually use daily. Complexity and inconvenience are the top reasons people abandon at-home health devices.
Best Times to Use Red Light During Teeth Brushing
The most effective time to use red light therapy is immediately after brushing and flossing, not before.
Clean gum tissue absorbs light more efficiently because there’s no biofilm or debris acting as a physical barrier between the light source and the tissue. Think of it like applying sunlight to a clean window versus a dirty one.
For people using an integrated red-light toothbrush, this is handled automatically since the light activates during the brushing cycle itself. For standalone mouthpiece devices, building the habit of using it as the final step in your oral care routine is the most reliable approach.
It’s a tad easier to remember to use it in the morning, since most people are less likely to forget steps in their morning routine than at night when they’re tired.
However, there’s a good reason to use it at night: we produce less saliva when we sleep, which makes our mouths more acidic and bacteria-friendly. Using red light before bed means your gums will be ready to heal during their overnight repair cycle. If you can only do it once a day, pick the time you’re most likely to stick to.
How to Know Your Gums Are Healing
It is not always easy to tell when your gums are improving, but there are a few early signs people often watch for.
One of the first changes some people look for is less bleeding when they brush. Gums that used to bleed with light brushing may start to feel less reactive over time.
You may also notice less redness along the gumline, less puffiness, and tissue that looks firmer and calmer. Some people also find that the area feels less tender during brushing or when eating hot or cold foods.
If you’re tracking your gum health with a dental professional, changes in probing depths and overall gum assessment are the most reliable ways to monitor improvement.
Red Light Therapy Should Not Replace Regular Dental Checkups
It’s important to remember that red light therapy is a complementary treatment, not a replacement for regular dental checkups or a cure for serious oral health issues. Conditions like gum disease, cavities, and other serious oral health issues still require professional diagnosis and treatment.
No home device, no matter how advanced, can replace the deep cleaning, surgical procedures, or diagnostic capabilities of a dentist. Using red light therapy as an excuse to avoid regular dental checkups is not only counterproductive, but it can also be dangerous.
Where Red Light Therapy Fits in Your Oral Health Plan
| Role | Red Light Therapy | Professional Dental Care |
|---|---|---|
| Daily maintenance | ✓ Ideal — supports tissue health between visits | Not practical for daily use |
| Active gum disease treatment | Supportive adjunct only | ✓ Required — scaling, root planing, or surgery |
| Inflammation reduction | ✓ Clinically demonstrated benefit | ✓ Professional cleaning removes causative factors |
| Healing acceleration | ✓ Supports recovery after procedures | ✓ Provides the procedure itself |
| Diagnosis | ✗ Cannot diagnose conditions | ✓ Essential — X-rays, probing, visual exam |
| Pain management | ✓ Reduces soft tissue discomfort | ✓ Addresses root cause of pain |
The smartest way to use red light therapy is as the daily layer of support that keeps your gum tissue as healthy as possible between professional cleanings. When your gums are in better shape going into a dental appointment, the cleaning is less involved, recovery is faster, and your long-term trajectory improves. It’s the difference between managing your oral health proactively versus reactively.
Before incorporating any at-home device into your routine, especially if you are undergoing treatment for active periodontal disease, it is important to consult with your dentist or periodontist.
In most instances, they will be supportive, especially if they are familiar with the research on photobiomodulation, and understand its role as a supplementary tool. However, it is crucial for your provider to be aware of what you are using, so they can accurately incorporate it into your overall care plan.
FAQS on Red Light Therapy for Teeth and Gums
Can I Use Red Light Therapy in My Mouth Every Day?
Daily use may be reasonable only if the device is specifically designed for intraoral use and you follow the manufacturer’s instructions exactly.
Photobiomodulation used within appropriate dental parameters is generally discussed as low-heat and non-UV, but that does not mean every red light device is suitable for the mouth.
A general skincare panel should not be treated as equivalent to an oral device, and ongoing bleeding, pain, ulcers, or suspected infection should be assessed by a dentist.
How Long Does It Take to See Results From Red Light Therapy on Gums?
Results, when they happen, are usually evaluated over weeks rather than after a single session. Some people may notice early changes such as less bleeding or tenderness within a few weeks, but visible gum improvements and professionally measured changes generally take longer.
The timeline depends on the condition being treated, the device, the dose, and whether red light therapy is being used alongside standard dental care.
Is Red Light Therapy a Solution for Gum Disease?
Red light therapy is not considered a stand-alone treatment for gum disease.
Current dental research mainly discusses photobiomodulation as an adjunct, meaning it may support healing or help with inflammation when combined with plaque control, scaling, and professional periodontal care. Persistent bleeding gums, loose teeth, bad breath, or gum recession still need a dental evaluation.
Can Red Light Therapy Make My Teeth Whiter?
Red light therapy does not have good evidence as a teeth-whitening treatment on its own. In dentistry, whitening is typically achieved with peroxide-based bleaching systems or other dedicated whitening methods, while photobiomodulation is more often discussed in relation to sensitivity, healing, or comfort. Claims that standard red light exposure alone whitens teeth should be treated cautiously.
Disclaimer: This content is for informational purposes only and does not constitute medical or dental advice. Red light therapy is not a substitute for professional dental care, diagnosis, or treatment. Consult your dentist before using any intraoral red light device, especially if you have bleeding gums, pain, infection, ulcers, recent dental work, or an existing oral health condition.